Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsBappenas, UI modeling shows grim projection of COVID-19 spread in Indonesia
Change text size
Gift Premium Articles
to Anyone
I
f Indonesia does not step up its current COVID-19 control measures, the country might have to deal with a "collapsed" healthcare system and hundreds of thousands of deaths, as shown by a projection by the National Development Planning Board (Bappenas) and the University of Indonesia's (UI) public health experts.
The modeling indicates that without mandatory physical distancing and mass testing, categorized in the document as a high degree of intervention, the country could see between 47,984 and 240,244 deaths without taking into account medical and treatment intervention.
Even with such drastic mandatory measures, the virus could infect some 500,000 people and kill 11,898 people, while the absence of intervention might lead to some 2.5 million positive cases by April.
The figures merely refer to cases needing hospital treatment, with forecasts based on the assumptions that the doubling time in Indonesia is four days and that each case could infect at least two other people.
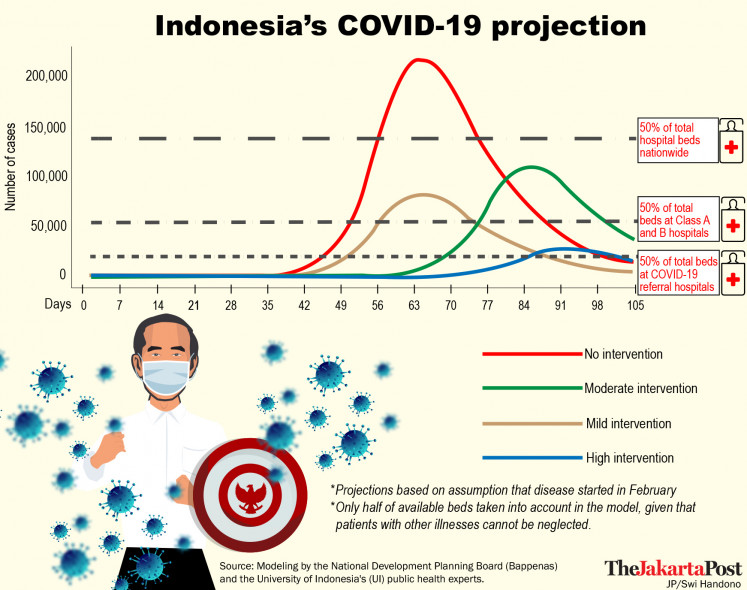
Indonesia's COVID-19 Projection (JP/Swi Handono)This has raised concerns that the highly contagious virus will, if it has not already, take a toll on hospitals in the country, which only have 8,158 ventilators and 105 isolation rooms with ventilators nationwide, according to data from the Health Ministry that was cited in the Bappenas documents.
The figure excludes the ventilators and isolation rooms provided at a former athletes village in Kemayoran, Central Jakarta, which has been turned into an emergency hospital to treat people with COVID-19.
"It is a projection based on assumptions, and in this case it depends on the scenario,” Bappenas director for public health and nutrition Pungkas Bahjuri Ali told The Jakarta Post on Sunday. “The figures will of course be different if a different intervention is adopted. The better and more massive the intervention, the lower the number of cases will be.”
Rather than starting the modeling from March 2, when Indonesia announced its first two confirmed cases, it started from February given the high likelihood of cases being undetected and is based on surveillance data from the Jakarta Health Agency. Jakarta is now deemed the country's epicenter with 698 confirmed cases and 78 deaths.
Pungkas said that based on the projection, his office had recommended mandatory social distancing to the government.
On Monday, President Joko “Jokowi” Widodo instructed his aides to draft a clear regulation to act as guidance for regional administrations in implementing large-scale social distancing, although he added that the final decision on quarantine measures rested with the central government.
Read also: Jokowi orders large-scale social restrictions coupled with 'civil emergency' policies
A draft government regulation on health quarantine, a copy of which was obtained by the Post, however, does not stipulate sanctions for those failing to abide by the social-restrictions order.
Referring to the projection's intervention scenarios, the government was still engaged in no to moderate intervention, meaning that physical distancing remained voluntary by restricting mass gatherings without mass testing, said Pandu Riono, one of the UI experts who was involved in the Bappenas project.
If this went on, the number of cases would exceed hospitals' capacity by April, in this case 50 percent of the beds at the 132 COVID-19 referral hospitals and 50 percent of the beds at class A and B hospitals, which are mostly centered in Java. Only half of the beds were taken into account in the model, given that patients with other illnesses could not be neglected by hospitals.
By the end of April, a similar result would take place even if the government was engaged in moderate intervention through voluntary physical distancing and small-scale mass testing.
With stricter physical distancing measures and mass testing, however, the number of cases would only exceed the 132 referral hospitals' beds by early May, the modeling shows.
Read also: Some 70,000 Indonesians could be infected with COVID-19 before Ramadan, scientists say
Pandu said the government was left with "no other option" than to impose sanctions on those violating mandatory physical distancing, such as by imposing community quarantines, as well as mass polymerase chain reaction (PCR) testing, given that rapid testing was insufficient to detect cases as early as possible.
Indonesia has tested some 6,500 people so far and recorded 1,414 cases with 122 deaths in less than a month since it announced the first confirmed cases.
The high fatality rate is largely due to the late detection of cases and limited hospital capacity, Pandu said, urging the government to start "resource-mapping for this war".
This included using the country's existing test kits for tuberculosis that could be modified and used for COVID-19 with adjusted cartridges, as well as importing more PCR test kits and empowering more laboratories, he said.
He added that medical workers, a growing number of whom had been infected by the virus, must be protected as Indonesia’s ratio of doctors to population was low and unevenly spread between regions. Research by the World Bank in 2017 showed that Indonesia had only four doctors per 10,000 people.
"What happens now is the result of a messy [healthcare] system. This is a test of what [the government] has been doing so far, and what it shows is the inequality of [healthcare] services [across the country]," Pandu said.
Read also: Indonesian government could use TB test kits for COVID-19, doctor says
The government spokesperson for COVID-19 affairs, Achmad Yurianto, said the government would make use of PCR machines, commonly found at referral hospitals and which were previously used to detect tuberculosis, to run samples from the modified tuberculosis test kits.
The government will also import COVID-19 test kits from the United States, which has been using the same method; starting with 100 kits this week for training and machine-setting purposes.
"We will order 10,000 [kits] next and 112,000 are currently in the manufacturing process," Yurianto told the Post on Monday, adding that it would take three to four hours for the results to be known.