Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsFor all citizens or only the poor?
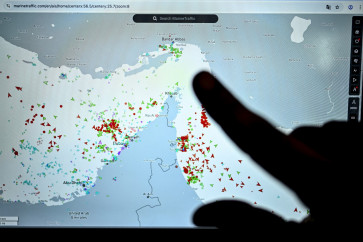
Patients queue for health services at Pasar Rebo Hospital, East Jakarta, in May
Change text size
Gift Premium Articles
to Anyone
Patients queue for health services at Pasar Rebo Hospital, East Jakarta, in May. (JP/P.J. Leo)
For Jakarta's citizens, the KJS program improves on the Health Services for Poor Families (JPK Gakin) program.
Despite ongoing glitches on services, the health plan has covered more citizens, not only the poor.
The universal scheme, however, has caused confusion among residents and officials, even Jokowi.
Jakarta Legislative Council member Neneng Hasanah, said some low income residents in West Jakarta have been denied service by hospitals, while other who are financially more capable have benefitted.
At least Gakin targeted the poor, the Democratic Party councilor says. 'Now, it's difficult to distinguish who is entitled to free health care.'
The KJS system is open to abuse, she says, adding that the city should reevaluate its policy and tightening the criteria for defining 'poor.'
Yayasan Demokrasi Jakarta, a foundation advocating healthcare access for marginalized people, says KJS patients have been rejected.
Other KJS participants have been required to leave deposits before receiving a treatment, says Muhammad Agus, head of the Democratic Party-affiliated foundation. 'They never saw their money back.'
Governor Joko 'Jokowi' Widodo tightened criteria after critics said that KJS was missing its target. The new rule referred to Gakin criteria for defining the poor and excluded those with existing health insurance, such as civil servants.
However, imposing the criteria has been easier said than done. Community health centers, which register participants and issue KJS cards, have no way of determining if an applicant is poor.
Further, some civil servants ' who are already covered by government-run Askes health insurance ' prefer all-costs-paid KJS coverage.
Although state-owned PT Askes helps administer the KJS system, its database does not indicate if a participant is already covered under its health scheme.
Jokowi also has required that all KJS patients first visit their local community health centers for referrals for hospital treatment is required.
After the initial euphoria over KJS, patient numbers have eased, if only a little. Budhi Asih General Hospital, for example, saw its daily patient intake double to 1,000 when the KJS was launched; this has since fallen to 800.
Hospital spokesman Hamonangan Sirait says KJS hospitals have imposed additional criteria, such as limiting daily general healthcare coverage to Rp 500,000 (US$40.93), with no prescriptions for vitamins.
For budgeting, Jakarta uses a figure of 4.7 million participants, or half the city's population, each of whom has a monthly premium of Rp 23,000 paid by the city, resulting in an annual allocation of close to Rp 1.3 trillion for 2013.
Each hospital receives a monthly allocation based on its number of KJS participants, and they have to file a periodic spending report of with the help of PT Askes.
Unlike as in its national program, Askes does not handle financial transactions between the government and hospitals under the KJS. Its role is limited to administration.
'We verify and cross check hospital claims,' says Irfan Humaedi, head of Askes public relations.
While Askes has set up offices or assigned staff at participating hospitals, confusion about the KJS program remains.
Problems do not seem to be structural; rather they appear to be teething pains. One constraint is that people do not know how the system works.
Some have heard of the KJS, but do not know that they must register, turning up at hospitals demanding immediate service, says Theryoto, the head of the city Regional Health Security Unit.
Patients aren't the only ones ill-informed about the KJS. Community health centers, on the frontline of the healthcare system, also have difficulties informing the patients of their rights and obligations.
Erika, who runs a health center in West Jakarta, suggests that the city government launch a more thorough public information campaign about the KJS.
'Often I am as clueless as the patients. I feel stupid,' she says.