Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
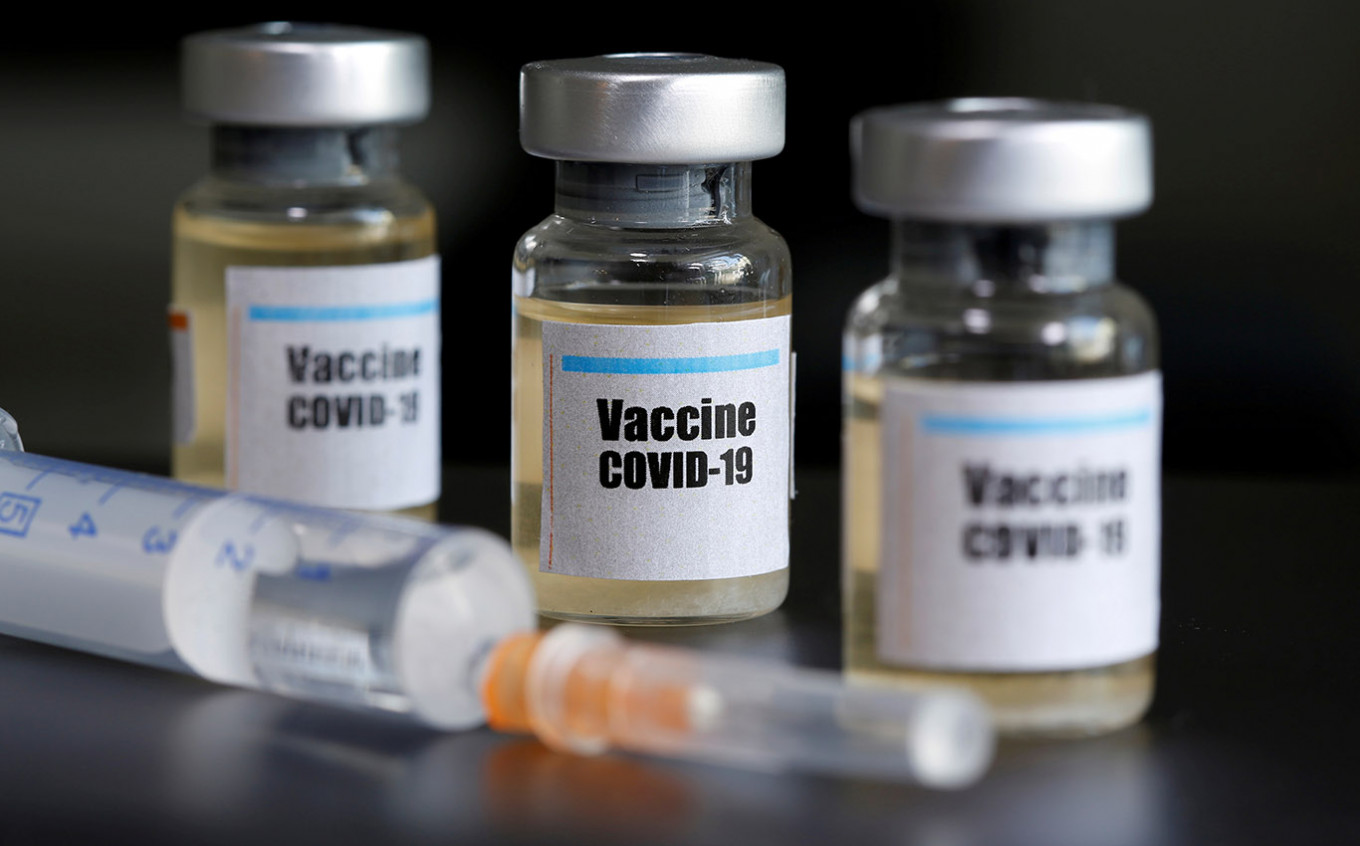
View all search resultsIndonesia targets local COVID-19 strain in Eijkman-led 2022 vaccine initiative
Joining scientists and researchers around the world in the global race to develop a COVID-19 vaccine, Indonesia has launched a government initiative that aims to develop a vaccine that specifically targets the coronavirus strain in the country.
Change text size
Gift Premium Articles
to Anyone
I
ndonesia is looking to fast-track the local development of a COVID-19 vaccine, but concerns remain as to whether insufficient funding and facilities, as well as the country's reliance on imported materials, might hinder the initiative.
The government has appointed the Eijkman Institute for Molecular Biology to spearhead the vaccine development program through a consortium that includes the Health Ministry's Research and Development Agency (Balitbangkes), state-owned pharmaceutical company PT Bio Farma and several universities.
The institute has been given a time frame of just 12 months starting in April, Eijkman director Amin Soebandrio told The Jakarta Post on Sunday.
Vaccines typically require 10-15 years to develop through several stages, including clinical trials and licensing for national immunization programs, according to the United States' CDC.
Eijkman will send any prototype seed viruses it produces – the "seed stock" needed to manufacture vaccines, also called candidate vaccine virus (CVV) – to Bio Farma, the country's sole vaccine manufacturer, for accelerated clinical trials on human volunteers. According to the plan, Bio Farma aims to mass-produce the vaccine by 2022.
This was much faster than the typical five to 12 years needed for vaccine development, said Bio Farma R&D manager Neni Nurainy.
Challenges ahead
Amin said that the target was not impossible, but that the accelerated process would have its own share of challenges, particularly in terms of facilities and funding.
Eijkman has received Rp 5 billion (US$329,989) for the exploratory stage of vaccine development. The sum is part of Rp 90 billion in total funding that the Research and Technology Ministry has budgeted for the consortium's COVID-19 studies.
"If we count everything, [the fund] might not be enough, but we can make use of existing resources and [testing] kits. We are not starting from zero,” Amin said.
Research and Technology Minister Bambang Brodjonegoro said that the funding for Eijkman "will be added to as necessary". He was also well aware that Bio Farma would require large funds to manufacture the vaccine to provide coverage for the country's 260 million people.
Another challenge, Amin said, was that Indonesia still needed to import reagents for the COVID-19 tests at a time when the pandemic had disrupted the global supply chain.
Bio Farma's Neni expressed the same concerns. "There must be support from all parties to accelerate [vaccine] development, [including] funding, raw material procurement, regulations and capable researchers," she said.
Exploratory stage
As coronaviruses mutate easily during replication to adapt to its host, the vaccines developed in other countries might not be viable against the strain in Indonesia, Amin explained.
Eijkman's laboratory has been conducting whole genome sequencing to determine the complete RNA sequence of the SARS-CoV-2 strain in Indonesia. This is part of the initial stage of vaccine development.
Scientists will then be able to detect the antigen of the Indonesian strain and identify the strains in other countries that share the closest genetic traits. In other words, the scientists will trace the chain of transmission of the Indonesian strain.
Given Indonesia's vast archipelagic geography, Amin said that the Eijkman lab would need to collect samples from several regions, which would be a challenge in itself. This would ensure, however, that the CVV it prepared would be suitable for mass-producing a vaccine for immunizing people across the country.
"That's why we have to make [the vaccine] specific [to the Indonesian strain]," he stressed. "Although we can identify the parts of the virus that don't [mutate], the antigen that is discovered might not be good enough for developing into a vaccine."
Many institutions around the world have been sharing their genome sequences of local coronavirus strains with global databases such as GISAID and Nextstrain.
Eijkman on Monday submitted its first three complete genome sequences of the Indonesian strain to GISAID. This was the first submission from Indonesia, although the Health Ministry's lab announced that it was also sequencing the virus early in the outbreak.
Aside from developing a vaccine, genome sequencing can also help with contact tracing. Amin said that the lab was still analyzing the possible origin of the virus strain in Indonesia.
Once the antigen is detected, the Eijkman lab will formulate a vaccine prototype for animal testing with other members in the consortium.
Bio Farma's role
Following successful animal testing, the vaccine seed will then be given to Bio Farma for clinical trials. If the vaccine seed passes the clinical trials, the company will start mass-producing the vaccine.
Neni said it was too early to estimate the amount of vaccine the company would be able to produce by then.
While clinical trials generally took years, said Neni, the final two phases of the clinical trial could be run in parallel to cut time during a health emergency.
Once the safety and efficacy of the vaccine had been proven, the vaccine could be approved for mass distribution under supervision of the Food and Drug Monitoring Agency (BPOM).
Solidary Trial, other options
While there is still a long way to go until a vaccine is available in the country, 22 Indonesian hospitals have joined the World Health Organization (WHO) Solidarity Trial that coordinates clinical trials for potential antiviral treatments.
The program is running comparative trials on four possible treatments: remdesivir, lopinavir and ritonavir, a combined treatment of lopinavir-ritonavir with interferon beta-1a, and chloroquine or hydroxychloroquine.
The WHO and the Health Ministry is providing the untested drug treatments to the enrolled hospitals. The ministry has supplied the treatments to at least eight hospitals by April 23, five of which were ready to recruit volunteers and start randomized clinical trials.
Jakarta's Persahabatan Central General Hospital is among the 22 Solidarity Trial hospitals in Indonesia.
Spokesperson Erlina Burhan said that the hospital had yet to receive the treatments and was still preparing for running the trials. She said that the hospital had been treating COVID-19 patients according to a protocol created by medical organizations.
A copy of the protocol that the Post obtained suggests the use of several drugs for COVID-19 treatment: the antimalarials chloroquine phosphate and hydroxychloroquine, the antiviral oseltamivir (Tamiflu) that has been used to treat bird flu and the experimental antiviral favipiravir (Avigan) that has been used to treat Ebola patients.
Indonesian researchers are also looking at other alternative therapies, including the use of convalescent plasma from recovered COVID-19 patients for treating current patients that have developed a severe form of the disease.