Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsCOVID-19 surveillance remains lacking in Indonesia
Change text size
Gift Premium Articles
to Anyone
I
ndonesia is in a race against time to contain the COVID-19 outbreak as patients overrun health facilities and medical workers are overwhelmed, but primary efforts to break the chain of transmission are still far from expected, epidemiologists say.
Testing, tracing and isolation are key to containing COVID-19. But these measures remain weak in Indonesia, largely because of limited testing capacity, an insufficient number of COVID-19 tracers and people’s reluctance to open up to these workers.
On Oct. 7, a total of 44,212 specimens from 32,167 people were tested, according to the Health Ministry. On the same day, the ministry recorded 142,213 suspected cases. No data is available on the number of probable cases.
Suspected cases are those with acute respiratory illness who have recently traveled or been exposed to a confirmed case, while probable cases are suspected cases with severe symptoms clinically consistent with COVID-19.
Both still have no laboratory evidence, but probable cases also include those with inconclusive test results.
Indonesia currently has 376 laboratories with a combined testing capacity of around 40,000 specimens in a day.
Masdalina Pane of the Indonesian Epidemiologists Association (PAEI) said that having a high number of suspected cases on the waiting list for diagnostic tests would definitely delay contact tracing, quarantine and treatment. She said health authorities should reduce testing turnaround times and deploy more tracers or use more volunteers for COVID-19 surveillance.
“Having no conclusive diagnostic status is a big problem. But if the capacity of labs remains limited, [health authorities] should make priorities on who to be tested -- preferably probable and suspected cases with severe symptoms and they should get the lab results within 24 hours,” she said on Wednesday.
COVID-19 testing in Indonesia is at 70.13 percent of the World Health Organization (WHO) benchmark of one per 1,000 people per week, according to the government's COVID-19 spokesman Wiku Adisasmito on Tuesday.
Read also: Contact tracing the missing link in Indonesia's battle with COVID-19
On Thursday, Wiku said the main reasons why to date Indonesia had yet to meet the benchmark were the limited number of tracers and supporting facilities, difficulties in reaching out to all contacts due to Indonesia's vast and scattered regions, as well as persistent COVID-19 stigma.
Wiku called on local health authorities to strengthen the role of Puskesmas and the public to report to health authorities about their history of contact with confirmed or suspected cases.
“We need the help of people to report their own history of contact with known cases,” he said.
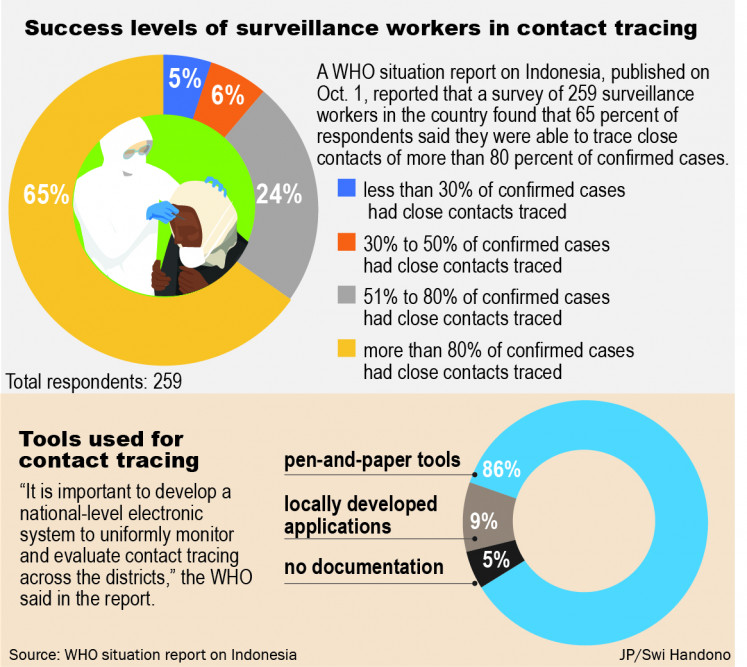
A WHO situation report on Indonesia, published on Oct. 1, reported that a survey of 259 surveillance workers in the country found that 65 percent of respondents said they were able to trace close contacts of more than 80 percent of confirmed cases.
The report said, based on a focus group discussion with surveillance-related stakeholders held in East Java last month, the main issue that was still looming over contact tracing was the stigma surrounding COVID-19. Limited numbers of traces was another problem, the report said.
Masdalina suggested authorities strengthen the role of community health centers (Puskesmas) as they are the most capable to perform tracing adequately.
Puskesmas are the backbone of public health across the nation, particularly in remote areas. But as they struggle with a lack of tracers, Masdalina urged them to recruit local residents to help with tracing efforts.
“Local communities usually have appointed their own health volunteers, who can be trained and help Puskesmas with contact tracing, rather than deploying people from nowhere and who have no basic knowledge on this,” she said.
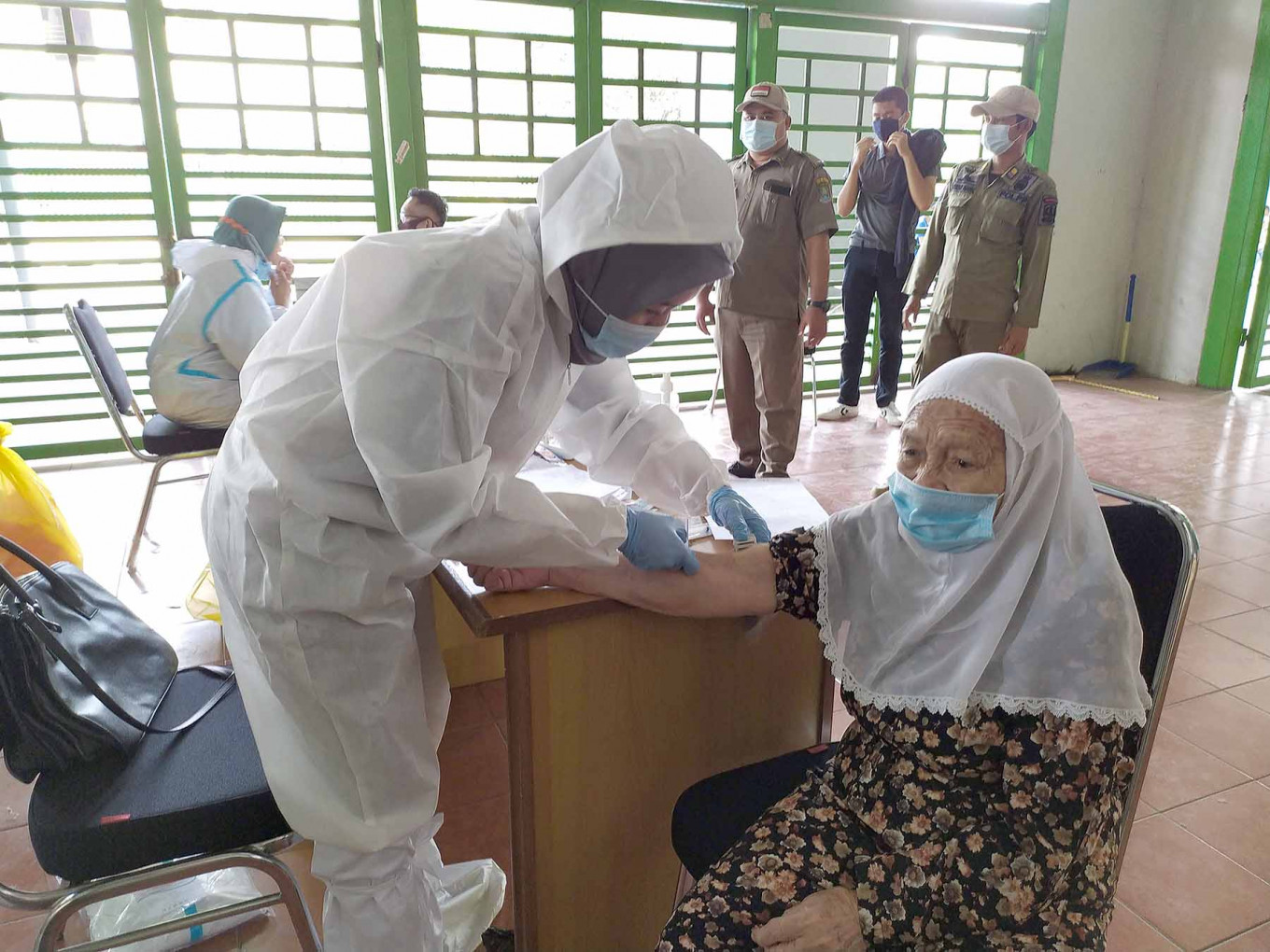
Indonesia currently has 376 laboratories with a combined testing capacity of around 40,000 specimens in a day. (JP/Swi Handono)Epidemiologist Dicky Budiman from Australia's Griffith University said efficient reporting and data collecting of tracing results also matter much -- otherwise, containment would fail and cases would continue to multiply.
For many health surveillance workers in the country, tracing is laborious work, as 86 percent of the workers surveyed revealed they still used paper-based methods, while only 9 percent used locally developed applications, the WHO report said. The remaining 5 percent did not document the procedure.
Maulidiya Muliawati, 23, a health volunteer at Puskesmas Grogol Petamburan in West Jakarta, said she was primarily assigned to promote health awareness. But lately she has been helping surveillance workers to input data due to a heavy workload in contact tracing.
“It took me around 2.5 hours to input data from around 30 questionnaires into one platform,” she said recently, adding that the work for surveillance officers requires them to input data into at least five different platforms, including on a website and a spreadsheet.
“It could be hundreds on busy days,” she added.
Due to the manual work, the WHO report said “it is important to develop a national-level electronic system to uniformly monitor and evaluate contact tracing across the districts”.
“There is no other way [to contain COVID-19] than improve testing and tracing capacity [...] We could have found more [people infected with the virus] with a more effective process,” Dicky said.