Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
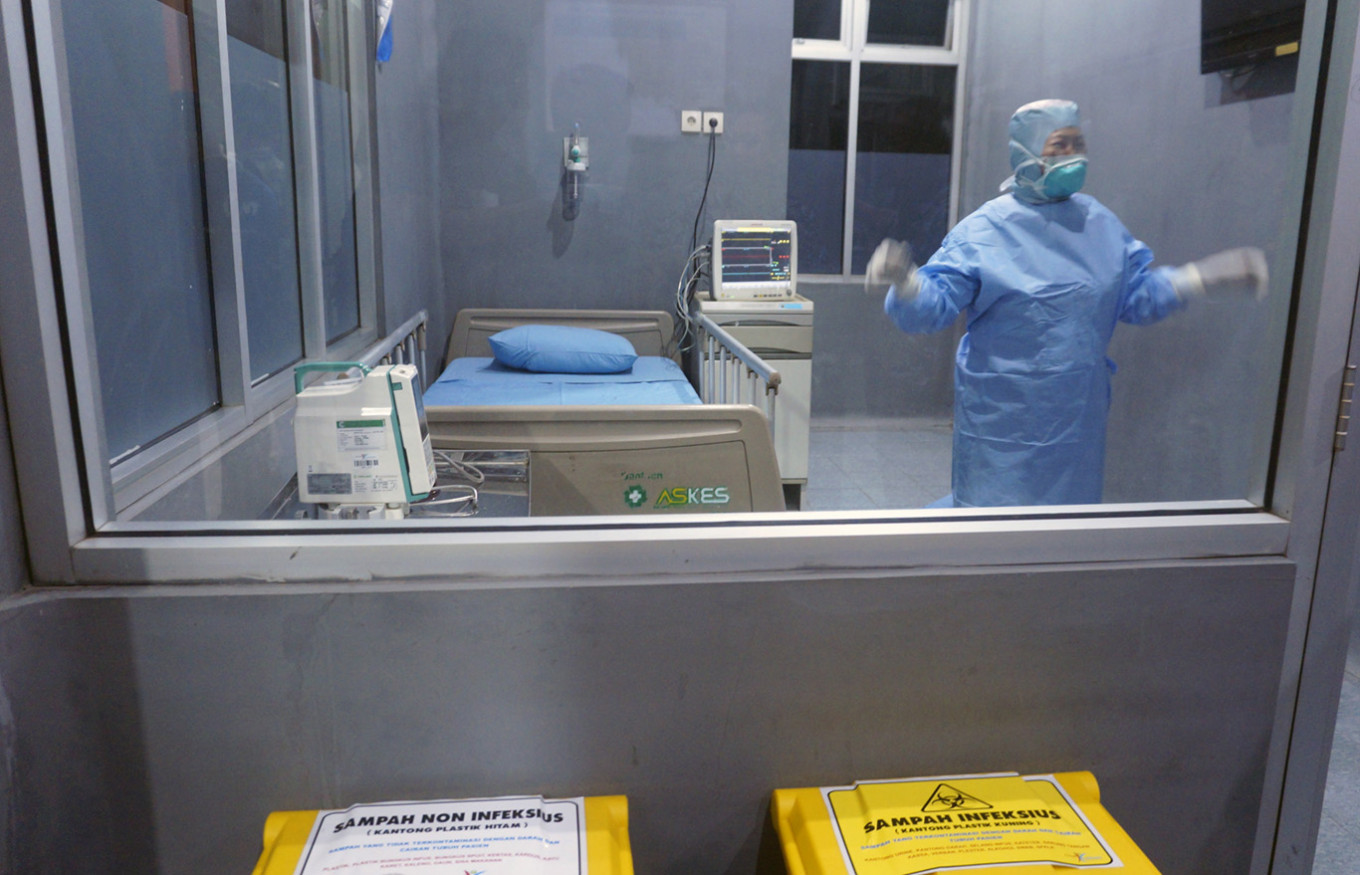
View all search resultsCOVID-19 response must incorporate TB, malaria, HIV programs as essential services
Indonesia cannot afford any delay in its extant healthcare programs for tuberculosis, malaria or HIV/AIDS, and should instead consolidate its COVID-19 response to maintain these essential health services.
Change text size
Gift Premium Articles
to Anyone
T
he COVID-19 pandemic arrived suddenly to strike almost all countries in the world. The urgency to stop the pandemic has engendered unprecedented international effort and collaboration. While the focus is on controlling the pandemic, however, other extant epidemics are at risk of being abandoned.
For decades, the international community has been working together to eradicate tuberculosis (TB), HIV and malaria, but has yet to claim complete victory. TB infects 1,020,000 people each year in Indonesia. The HIV transmission rate in Indonesia is at an all-time high; malaria still hampers people’s lives in rural areas.
TB, HIV and malaria can lead to death and permanent disabilities. Tuberculosis mainly infects the lungs, but may spread to other organs. HIV weakens the immune system, which causes people living with HIV (PLHIV) to contract infections that are harmless in healthy people. Malaria may cause severe brain damage, kidney failure and chronic anemia, which is debilitating and can cause death or disabilities.
The focus on COVID-19 could cause reduced quality of other health services and programs. Severe disruption to regular services may be seen as a result of movement restrictions, diverting the healthcare workforce to COVID-19 response and disruptions to the pharmaceutical supply chain. The efforts to curb TB, HIV and malaria will decline as active case finding (ACF) programs stall and patient retention is hampered.
Minimizing any disruptions to prevention and treatment programs during the COVID-19 response is pivotal in a country like Indonesia that has a high burden of tuberculosis, malaria and HIV/AIDS cases. Failure to do so could lead to catastrophic loss of life.
Impacts of COVID-19 on tuberculosis
All healthcare facilities have implemented efforts to optimize passive case finding (PCF) for tuberculosis. Meanwhile, ACF is carried out by targeting high-risk groups based on risk network referrals from puskesmas (community health centers). In principle, both drug-sensitive and drug-resistant TB patients with mild to moderate symptoms can receive outpatient care, while hospitalization is required for those who present severe manifestations of the disease.
Puskesmas and hospitals are high-risk locations for COVID-19 transmission, so it is highly possible that patients are refraining from visits for fear of contracting COVID-19. High-risk clients such as patients' families may find it inconvenient to be assessed by doctors at health facilities. This may also hold true for drug-resistant TB patients who must physically visit a health facility to received their daily injection, resulting in missed doses that will worsen their condition.
Hospitalized TB patients may experience respiratory failure, which usually need a ventilator to help them breathe. They must share the limited supply of ventilators with COVID-19 patients who have developed respiratory failure. The mortality rate is significantly higher in patients whose need for a ventilator cannot be met.
In 2017, more than half of Indonesia were declared malaria-free. However, the risk of malaria still looms in eastern Indonesia. Aggressive vector control, case investigation, surveillance and case management are required to achieve malaria-free status in the region.
To prevent transmission of malaria, insecticide-treated bednets should be made available to all households and medication to infected people. Keeping people healthy by blocking the mosquito vector that spreads the malaria parasites and preventive treatment to eradicate the parasites are the keys to malaria control.
Most cases of malaria occur in Papua, East Nusa Tenggara, Maluku and West Papua. All four provinces have weak health system resilience because of their low numbers of health facilities and health workers. The COVID-19 crisis will likely render these local health systems vulnerable to disruptions to their malaria program.
In normal conditions, HIV case finding in Indonesia is conducted through mobile HIV testing programs that capture potential HIV-positive clients in hot spots such as red-light districts and gay lounges. These programs have been temporarily suspended because of the pandemic, however, and voluntary HIV testing at health facilities has dwindled. The movement restrictions might help slow infection if implemented correctly, but otherwise, high-risk sexual activities that can transmit the virus may still be going strong in the background.
PLHIV need a constant supply of antiretroviral (ARV) drugs that they must take every day. The COVID-19 pandemic has adversely affected Indonesia’s ARV supply chain, as the drugs are all imported. ARV stock is currently low in several provinces.
Furthermore, the movement restrictions may limit access to health services for PLHIV to refill their ARV prescriptions. PLHIV may also be afraid to keep their appointments at hospitals and puskesmas because of their high vulnerability to contracting COVID-19.
The low domestic supply of ARV and restricted health service access will in turn pose a threat to the wellbeing and health of PLHIV. Being unable to take their daily ARV dose can be deadly, as PLHIV may contract other diseases, including TB and COVID-19.
The decline in quality found in several epidemic control programs may mean a relapse in their hard-won progress. Health facilities must adapt and provide differentiated, patient-centered care. Patients should have easier access to healthcare services during the pandemic.
Several ideas have been explored and implemented in private settings: Telemedicine can provide remote medical consultation to patients; drug delivery services are now available in several cities in Indonesia. Beyond these, health authorities should institutionalize and endorse remote drug dispensing systems to provide a sufficient supply of medication so patients can improve and maintain their health.
Patients in Indonesia are heavily concentrated at public hospitals and puskesmas, so these facilities must have the flexibility to adapt to the current conditions. Jakarta has started ARV home deliveries for patients who are unable to visit health facilities in person. The government needs to intensify its effort and expand ARV delivery services to all regions.
The Health Ministry must formulate protocols for maintaining essential health services during a pandemic as a basis for local administration to stay on top of other disease control programs. Central-local consolidation must be enhanced. Above all, Indonesia must ensure the provision of essential drugs and health services to all, as TB, malaria and HIV prevention and control cannot be postponed.
***
Afifan Ghalib Haryawan is a graduate of the University of Indonesia medical school and works as a physician with Linkages, USAID's global HIV/AIDS project; Melani Ratih Mahanani is a graduate of Sebelas Maret University (UNS) and physician who works at the Epidemiology of Transition research group of the Heidelberg Institute of Global Health in Germany.