Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
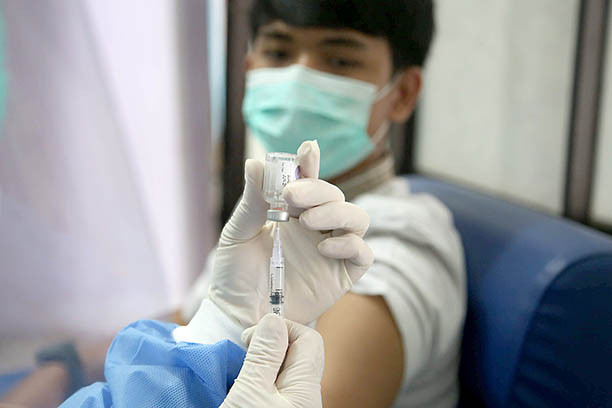
View all search results[INSIGHT] What we know so far about COVID-19 vaccines and new variants
Change text size
Gift Premium Articles
to Anyone
A
coronavirus, unlike some viruses that transform us into lifelong carriers (like herpes, or HIV), can actually be eliminated by our body.
Zania Stamataki, a researcher in viral immunology and senior lecturer from University of Birmingham explains that we have two different types of defenses that account for speedy and accurate action against a virus invasion. The defenses can be performed by our skin, saliva, tears, mucus, cilia (tiny hairs), stomach acid, urine flow or “friendly” bacteria, as well as army of white blood cells. These rapid defenses can be recognized when we suffer from the onset of sickness (fever, pain, redness).
The second type of defense accounts for accuracy that develops slower; it comprises B cells and T cells (called “immune cells”). T-cells act like powerful serial killers that instruct virus-hijacked cells to self-destruct via a “kiss of death”, so the viral load in your body can eventually be reduced. T-cells also leave memory cells behind. Pre-existing specific T-cells that are likely to be remnants from a previous coronavirus that caused seasonal colds (not COVID-19) may explain milder infections in some people.
B-cells are antibodies that recognize a virus by remembering the different parts of different germs. Once memory B-cells are activated and pinpoint a certain virus like COVID-19 and its location, a particular antibody specific to that virus can be intensively produced.
This production takes days to weeks, but the produced antibodies and memory B-cells will persist after the virus is gone. That being said, your body can react rapidly and neutralize the virus without your developing severe symptoms when you get a later infection from the same virus.
So, the point of vaccination is to give rise to potent antibodies that provide us with protective immunological memory. History shows that vaccines have been able to eradicate infectious diseases from the planet (for example, smallpox).
Pfizer and Moderna use messenger RNA/mRNA-based technology as their main ingredients in vaccines. As we know mRNA is a type of molecule whose job it is to transport copies of genetic instructions (imagine a shopping list or recipe) around a cell to guide the assembly of “spike” proteins of the coronavirus. This mRNA is responsible for only a part and not the whole virus itself, thus it is harmless but sufficient to cause your body to react to it.
Pfizer also highlights that its vaccine is “preservative-free” or free of a known preservative named thimerosal that contains mercury to help kill contaminant bacteria in vaccine vials. This mercury-based preservative has long been troublesome around over whether vaccines cause autism. The Pfizer vaccine also does not contain microchips.
Language does matter when it comes to vaccines. It often frustrates scientists when the media does not appreciate or distinguish between terms.
Stamataki emphasized that the word “efficacy” is a carefully chosen word used to describe the performance of a treatment under ideal VS controlled conditions. For example, Pfizer reported 95 percent efficacy, which means its vaccine prevented COVID-19 symptoms for 95 percent of those who received the vaccine compared with a placebo group that received no vaccine or irrelevant/known vaccines that should not work for the targeted virus. For COVID-19, safe vaccines with an efficacy at least 50 percent are expected to be approved by the United States Food and Drug Administration.
According to The Lancet Pfizer and Moderna reported 94.5 percent efficacy in an interim analysis, AstraZeneca and the Oxford Vaccine Group reported up to 90 percent efficacy and an acceptable safety profile on their vaccine candidates.
How about vaccine effectiveness? This number will be unlikely to reach 90 percent and we do not know yet what the overall effectiveness of the vaccine will be in preventing COVID-19 symptoms, severe reaction to infection or death for several years ahead through observational studies (vaccine performance for different groups, i.e., age, ethnic backgrounds, other health conditions; duration of protection) said Stamataki.
A group of researchers from the Cambridge Institute for Therapeutic Immunology and Infectious Diseases has recently reported a new variant of SARS-CoV-2 (the coronavirus that causes COVID-19) that has possibly arisen due to immune-selection pressure in infected individuals. This new variant has increased infectivity, higher transmissibility and is responsible for a current surge in COVID-19 cases in the United Kingdom and some parts of Europe.
SARS-CoV-2 is an RNA virus with a mutation rate of nearly one mutation a month but with passing time, mutations accumulate, and the virus evolves to evade recognition by antibodies and immune cells by changing some part of its features. The mutation is driven by error-prone processes when the virus replicates, thus happening at random so one cannot predict if the virus that accumulates mutations overtime will be more or less dangerous/contagious.
Reassuringly, we can maintain surveillance to adapt our vaccines as we have tools to keep up with the new information of the virus using various genetic sequencing methods (i.e., changing the vaccine’s recipe). Continued emphasis on testing/tracing remains essential together with the vaccination efforts globally.
A vaccine is definitely not the end, and any antiviral drugs to treat COVID-19 are not a substitute for vaccination either. In addition to getting a COVID-19 vaccination shot, people should still take the same everyday preventive measures: wearing masks, covering coughs and sneezes, washing hands often, as well as minimizing physical contact to avoid getting infected and to prevent transmission.
----------
PhD student in environmental microbiology and biotechnology, King Abdullah University of Science and Technology, Saudi Arabia