Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsHPV vaccine for cervical cancer prevention: Yes or no?
Cervical cancer is the second leading cause of death by cancer for women in Indonesia after breast cancer. The relatively good news is that the cause of this cancer and its vaccine have been discovered.
Change text size
Gift Premium Articles
to Anyone
T
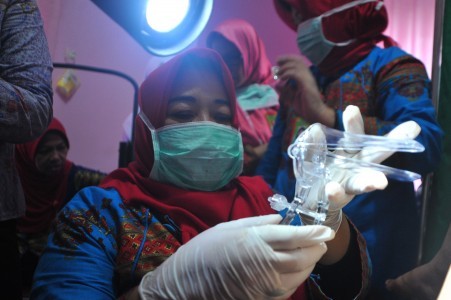
he Jakarta Health Office has conducted free and mandatory human papilloma virus (HPV) vaccination in various elementary schools for female fifth- and sixth-grade students aged 9 to 13.
The vaccine aims to prevent the human papilloma virus, which causes cervical cancer, from reproducing.
However, some parents have refused to allow their children to be vaccinated for several reasons. Among these is the fear of premature menopause and the news that the vaccine used in Indonesia is no longer administered in America and Europe.
“The vaccine is not used [in America and Europe] because they’ve found a new one,” explained Andrijono, an obstetrician and gynecologist lecturing in the School of Medicine at the University of Indonesia.
Although it has been substituted, the one currently in use, Gardasil, remains effective.
“It’s still effective and we can benefit from its good track record compared with the new one,” said Andrijono.
The other question frequently asked is why it is given to children rather than women already sexually active.
“It will just provide total protection if given to pre-adolescent children,” said Andrijono.
Widiastuti from the Jakarta Health Service confirmed this by saying that if administered to adult women, let alone sexually active ones, the protection would not be optimal and the expensive vaccine would be wasted.
Read also: What to know about the cause, symptoms of cervical cancer
The good news is that the source of cervical cancer and its vaccine have been discovered. In fact, the HPV vaccine has been in use in Indonesia for quite a long time, but its use was limited owing to its high price.
Widiastuti said the screening routinely conducted in the form of a pap smear and IVA (advanced stage) tests found one cervical cancer case in 1,000 women. Its incidence is estimated at 38,000 cases a year, with a death rate of around 80 percent (30,400 per year). Usually about 70 to 80 percent of cases are discovered after reaching an advanced phase. On average, after two years the survival rate is only 6 percent.
Cervical cancer is controlled by the primary means of using the vaccine and the secondary means of screening (pap smears and IVA). Widiawati said that screening did not yet cover all segments of society because of limited equipment and women’s reluctance to have themselves examined.
To reduce the ever-increasing number of cervical cancer cases, the Jakarta Health Office initiated the HPV vaccination of female children. This idea was later supported by the central government so that it became a national vaccination program with Jakarta as a pilot project, to be followed in Yogyakarta.
The children’s vaccination will optimally function by protecting cervical cancer vaccine recipients for the next ten years. Many Indonesian girls get married below the age of 19. “So if they’re vaccinated as senior high school students, we may be too late because some of them have married,” said Andrijono, who is also chairman of the Indonesian Oncological Gynecology Association.
Read also: Immunotherapy offers hope to lung cancer patients
Besides, vaccination at a young age has shown higher efficacy.
Andrijono, using comparative data of vaccinations carried out in Sweden, pointed out that a vaccine administered at aged below 17 resulted in over 75 percent effectiveness. At 9 to 13, it is enough to give the vaccine in two doses or two shots. At 14 to 45 three doses are required.
According to Andrijono, the HPV also causes cancer of the mouth, anus, penis and nasopharynx. HPV vaccine shots at the right ages are expected to lower the risk of contracting these different cancers.
Andrijono and Widiawati are not against women being independently vaccinated outside the HPV vaccination program. “But they have to pay the vaccine costs themselves if they are not included in the national program,” added Widiawati.
The vaccination program will not lead to a reduction in routine pap smears or IVA examination and if the program can be continued, the screening will even be optimized so as to reach far-off locations.
However, the screening method is sometimes too late in detecting the cancer, which normally leads to partial or total removal of the womb, leaving the patient unable to bear children.
“This vaccine is expected to reduce the number of women affected by cervical cancer in the future, as has already been achieved by countries that have had early implementation of similar HPV vaccination programs,” Widiawati said.