Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
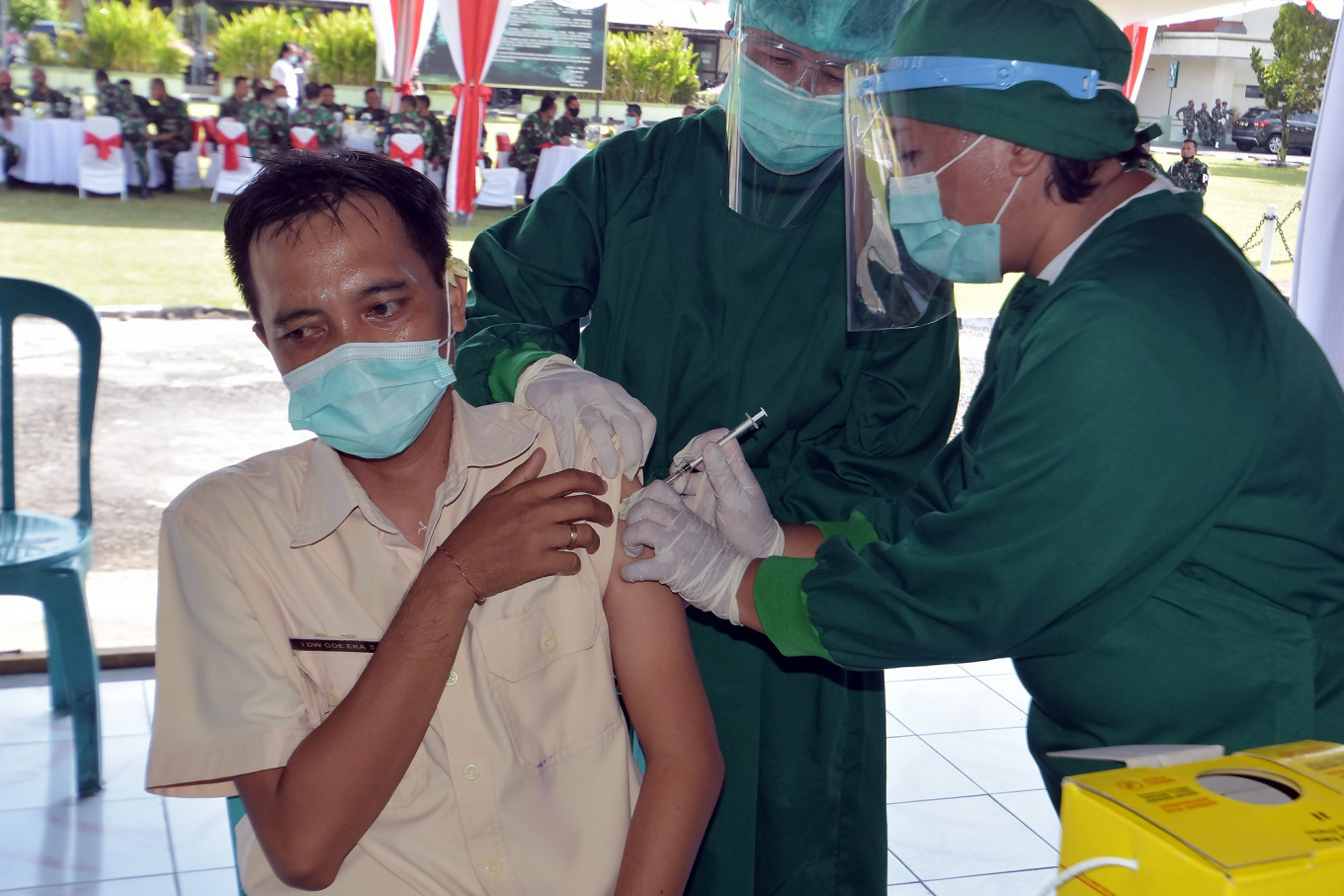
View all search resultsElderly people likely to be excluded from COVID-19 vaccination push
Vaccines all but guarantee that the people who get inoculated won't continue to spread the virus to others who aren't targeted in the vaccination program, such as the elderly, pregnant women and people with comorbidities.
Change text size
Gift Premium Articles
to Anyone
T
raveling home for the holidays is regarded by many Indonesians as part of a ritual of devotion and respect for their elders but when the current pandemic set in this custom was quickly turned on its head.
In Indonesia, there are at least 25 million people aged 60 years and above, categorized as the nation’s elderly.
They account for 10.4 percent of over 630,000 confirmed COVID-19 cases, but they also make up the largest share in the country's 19,000-plus fatalities at 39.3 percent, according to recent official data.
And while the studies are ongoing, the general idea is that the older you are, the higher the risk of developing severe illnesses when you are infected by SARS-CoV-2, the virus that causes COVID-19.
One Cabinet minister went as far as to say that people should not go home to their parents if they truly loved them.
But in spite of all of this, the elderly are not likely to be among the first to receive the COVID-19 vaccine, based on plans that Health Minister Terawan Agus Putranto revealed to lawmakers recently.
The reason for this has to do with the fact that potential vaccines are being trialed in the later stages only on people aged 18-59 years, as is the case with Chinese firm Sinovac’s CoronaVac, which is tapped for emergency use authorization in the near future, according to Terawan.
Experts are in agreement that the targeted age group for vaccination should follow available trial data, and that prioritizing certain groups of people is necessary given the limited availability of vaccines.
Priority groups typically start with frontline healthcare staff, essential service workers and people with health conditions that can lead to severe morbidity from infection. After that, immunization usually moves down the age groups from old to young, in line with case fatality rates.
Read also: Indonesia to cover only a third of COVID-19 vaccine recipients
Prioritizing productivity
Vaccines also might not work as well on the elderly, who commonly experience declining immunity as they age.
But some experts believe that the elderly should still be prioritized in the vaccination program, using candidate vaccines with proven efficacy and safety among this age group.
This means securing vaccine candidates from United States firms Pfizer and Moderna, both of which have reported efficacy rates well over 90 percent among test subjects over 65 years old, as well as the vaccine being developed by the United Kingdom’s AstraZeneca, which has generated similar results in immune responses across all adult age groups.
“The number of elderly people in the country is quite high, and I'm concerned about household clusters. I think they should also be prioritized, just like what the UK and the US are doing,” Indonesian Institute of Sciences (LIPI) biotechnology researcher Wien Kusharyoto told The Jakarta Post recently.
In 2019, a Statistics Indonesia (BPS) report revealed that 40.6 percent of elderly people in the country lived in three-generational households, meaning they lived together with their children and grandchildren. Another 27.3 percent of the elderly lived with other relatives.
Similar concerns were raised by Giovanni van Empel, a health policy specialist at crowdsourced database KawalCOVID-19, who said the big question that remained was how to ensure logistical efficiency so the vaccines could reach those people who really needed them.
Van Empel said it was “concerning” that some experts insisted the vaccines were there to protect the productive-age population so they could continue to work and eventually produce herd immunity, which depends on various factors.
For instance, just as Indonesia was about to roll out clinical trials for the CoronaVac vaccine in August, the trial’s research team leader, Padjadjaran University professor Kusnandi Rusmil, told the Post that “in order for people to remain productive”, those in the hardest-hit regions would need to get the vaccines first.
Researchers from Imperial College London have suggested that governments should aim to minimize mortality in the short term through vaccination, “unless vaccine supplies are short of what is required to protect the entire population for one year or more”.
In the case of the UK, vaccinating people over 70 would save more lives than focusing on those between 50 and 70 years old, given the steep rise in case fatality rates in the oldest age groups, they argued.
All but immune
Government officials have said that the aim of targeted immunization was to reach herd immunity. To achieve this, a certain portion of the population would need to be inoculated in order to keep people who do not get the vaccines safe from infection. Current estimates for the required coverage range from 60-75 percent.
In Indonesia's vaccination plan, the target is to inoculate 67 percent of the country's 167 million people aged between 18 and 59 years, which is 107 million people, around 40 percent of the country's total population.
Under this scheme, people outside the predetermined age groups will not get vaccinated, much like pregnant women and people with comorbidities. Altogether, they are expected to gain protection from herd immunity.
But doing so will not be easy or fast, experts have argued. The required coverage for herd immunity would depend on a vaccine’s efficacy and its reproduction number, which may vary across regions. Meanwhile, reaching that level of coverage would depend on supply and people’s willingness to get vaccinated.
Read also: Efficacy and effectiveness determine quality of COVID-19 vaccine: Task force
Current evidence also suggests that vaccines are geared toward preventing people from developing the disease or from getting infected, but whether it would stop transmission altogether remains to be seen.
This would mean that infected people who are inoculated could still possibly act as a vector and spread the virus, although some experts believe they would carry lower viral loads.
“That way, when someone is not infected, the infection rate can automatically slow down. But it doesn't mean transmission will stop completely,” Wien said.
Van Empel is more concerned that viral transmission among vulnerable groups who do not get vaccinated could technically still occur.
Back to basics
Terawan has said that the government could expand target coverage to other age groups once trial data and the vaccines themselves become available.
Based on data from US clinical trials database ClinicalTrials.gov, Sinovac has rolled out phase one and two clinical trials on healthy adults above 60 years since May, with results expected by the same month next year.
But as governments globally scramble to guarantee vaccination for their respective populations, Indonesia has only managed to secure some 160 million doses from Sinovac and US firm Novavax of the 246 million doses it needs to reach the target coverage. Officials say they are also in talks with Pfizer and AstraZeneca.
Much is also still unknown about the virus; the possibility of mutations cannot be ruled out, and it is unclear how long a vaccine may offer protection against the virus.
Global health researcher at Griffith University, Dicky Budiman, said that herd immunity through vaccination should be just one of many strategies that governments look at in their pandemic response.
The most important thing to do to keep people safe is to increase testing, contact tracing and quarantine, in addition to the state mantra of wearing masks, physical distancing and washing hands.
"The success of herd immunity through vaccination will also depend on these other containment efforts, because we have to push down the reproduction number as far as possible,” he told the Post recently.
“[In this sense] the elderly must – and have – the right to be protected.”