Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsThere's hope: No child should die from TB
Many developing countries still use the testing and treatment methods for tuberculosis developed 130 years ago, according to the STOP TB Partnership and the World Health Organization (WHO).
Change text size
Gift Premium Articles
to Anyone
T
he writer was invited by the International Union against Tuberculosis and Lung Health to attend the 49th World Lung Health Conference in the Hague and visit health facilities and research centers in the Netherlands under the media scholars program. The following is her report written to observe World TB Day 2019, which fell on Sunday.
Many developing countries still use the testing and treatment methods for tuberculosis developed 130 years ago, according to the STOP TB Partnership and the World Health Organization (WHO).
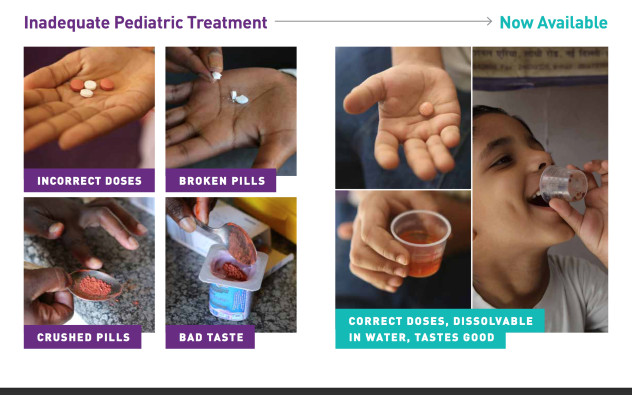
In the partnership’s “Towards Zero TB Deaths in Children” report it is states that the current vaccine for TB, the Bacillus Calmette-Guèrin (BCG), was discovered in 1920s and no new vaccine has become available since then. Worse, the TB treatment for children requires a mix of three to four different bitter-tasting and hard-to-swallow tablets over six months.
Currently, an estimated 239,000 children every year die from TB. Children with TB rarely die when they receive the standard treatment for the disease, but 90 percent of children who die from TB worldwide go untreated.
“No child should die from TB. There is an urgent need to drastically step up investment in research and development that can deliver new and better diagnostic tools,” said José Luis Castro, executive director of the Paris-based International Union against Tuberculosis and Lung Diseases.
Developing country: A mother sits with her child at the Kasangati Health Center on the outskirts of Kampala, Uganda. (Courtesy of The Union/-)
TB commonly affects the lungs, but in 20 to 30 percent of cases in children, it affects a different part of the body. Infants and young children are at special risk of having severe, often fatal forms of TB, such as TB meningitis, which can leave them blind, deaf, paralyzed or mentally disabled.
Currently, there is no simple, painless test for TB in children. A child must cough up a sample of sputum, which is then checked under the microscope for the bacteria that causes TB. Unfortunately, young children cannot spit up a sputum specimen and other methods are needed to get a sputum sample from them.
A doctor or health provider needs to insert a tube down the child’s throat and then inject liquid in order to get a sample to test. This is frightening and painful for any affected children.
New hopes emerged when a group of researchers at the KNCV Tuberculosis Foundation in the Netherlands shared their groundbreaking trial results during the World Lung Health Conference in the Hague in October 2018 in which a simple and low-cost method, using similar processing steps to those used for sputum, could diagnose TB at any GeneXpert site using stool samples.
This method was tested in vitro using TB-negative stool samples from children in Ethiopia, and on stool samples from 36 children with presumptive TB (pTB) aged below 15 years in a tertiary care hospital in Bandung, West Java.
The work is being conducted in collaboration with the Ethiopian and Indonesian research institutes and their respective national TB control programs.
“If further testing confirms the preliminary findings in Indonesia and Ethiopia, the potential for this method is enormous,” said Kitty van Weezenbeek, executive director of the foundation.
“Being able to diagnose TB and MDR TB from stools would mean that we have a method in our hands that can diagnose TB at the lowest healthcare level and can bring testing to hundreds of thousands of people,” she added.
”In that way, children can now get a microbiologically confirmed TB diagnosis at primary health centers, where that is currently not possible.”
The KNCV Foundation’s trial is one just many increasing efforts and advocacies made by scientists, donors, governments, the private sector and all stakeholders to address childhood TB at global and national levels and has brought the issue into the spotlight.
The childhood TB subgroup, established in 2003 as part of the Stop TB Partnership, began massive efforts and advocacy in response to the almost total neglect of TB among children within global and national TB control program activities and priorities.
The first achievement was the development and publication of the WHO childhood TB guidelines in 2006 and 2014 and the initiation of the first childhood TB meeting in Stockholm in 2011 followed by the publication of the first global estimates of TB in children in the 2012 Global Tuberculosis Report.
In October 2013, under the guidance of the childhood TB subgroup, now named the Child and Adolescent TB Working Group, the WHO and partners published the first Roadmap for Childhood Tuberculosis: Toward Zero Deaths, which laid out the strategic frameworks for the global fight against childhood TB aiming for zero deaths among children.
It also collaborated closely with the TB Alliance in the Unitaid-funded Speeding Treatments to End Pediatric Tuberculosis (STEP-TB) project to develop child-friendly fixed-dosed combination (FDC) medicine in 2015.
The Health Ministry in Indonesia – home to an estimated of 65,000 children with TB – has made significant progress in research, treatment, diagnostic, reporting, training and policy developments with support from the TB Care I project (2010-2015), Challenge TB (USAID-funded projects), the KNCV, WHO and Unicef and other organizations. (ste)