Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
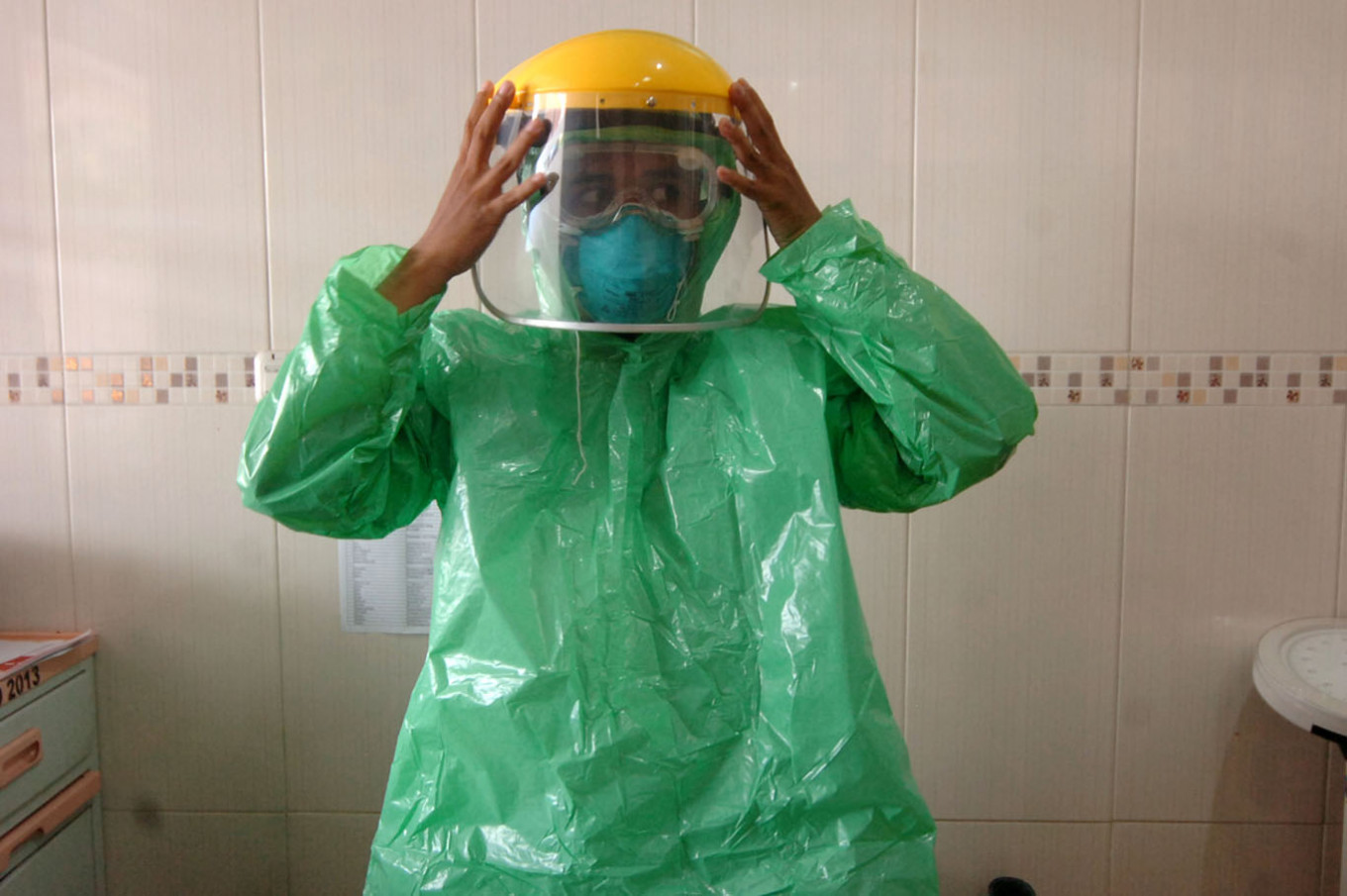
View all search resultsPPE production soars but quality, distribution issues remain
Change text size
Gift Premium Articles
to Anyone
Q
uantity does not equal quality for the Indonesian textile industry, which has contributed to a production surplus of personal protective equipment (PPE) to meet demand during the COVID-19 health crisis, despite complaints from users over quality and distribution.
The country now has the monthly capacity to produce 394.82 million surgical masks, an increase from just 150 million masks prior to the pandemic. As a result, Industry Ministry data project a surplus of almost 2 billion surgical mask by the end of the year.
The soaring production, which began in April, stemmed from the changing business in the textile industry during the pandemic and government demand due to prior supply shortages, Industry Minister Agus Gumiwang said on Tuesday.
“The textile industry was trying to sustain its factories by diversifying its products, which include surgical masks, cloth masks and coveralls. It led to significant growth of PPE production,” he said during an online discussion.
As demand dwindles, many textile industries are suffering from low factory utilization due to the government’s large-scale social restrictions (PSBB) to contain COVID-19.
As a result of the surplus, the Industry Ministry asked the Trade Ministry to revise a regulation that restricts the export of PPE so that it can begin exporting abroad.
“The oversupply condition must be addressed with the right policy to capitalize on the huge export potential for PPE,” Agus said, referring to Ministerial Regulation (Permendag) No. 23/2020.
However, national demand would still be prioritized, he said.
The nationally produced PPE include high-grade ISO 16604 standard coveralls for doctors and health workers at hospitals and AATCC 42 standard coveralls for test-site attendants, according to COVID-19 task force data.
The ministry projected a deficit only for N95 masks by the end of the year, when demand for the product is expected to surpass the actual number of produced masks by 5.39 million units.
Despite the industry’s success in avoiding PPE shortages, many health workers who are using the products are complaining about the quality of locally produced PPE.
“While the majority of the products have already passed the medical standards, many doctors are complaining that the coveralls are too heavy and uncomfortable. This is the reason why we could not take in all the locally made PPE products,” Health Ministry crisis center head Budi Sylvana said during the same discussion.
He added that many small hospitals and clinics also refused to use washable PPE and preferred instead to purchase disposable products, as they did not have the systems in place to disinfect PPE.
“There are cases of COVID-19 infection among medical workers that are caused by unsterile PPE. Not all hospitals have the ability to sterilize the PPE correctly,” he said.
Budi said small hospitals and clinics usually used a third-party laundry service that was not equipped with the tools for proper sterilization.
Besides being uncomfortable, Indonesian Hospital Association (Persi) secretary-general Lia Gardenia Partakusuma also complained about the distribution process of PPE to hospitals.
“Sometimes there’s a delay in PPE shipment due to a lack of supply, among other things. Hospitals need a steady supply of PPE to operate,” she said.
Persi data show that, on average, medical workers at 800 COVID-19 referral hospitals in Indonesia require 20 PPE per COVID-19 inpatient per day.
“As the PSBB are currently being relaxed, hospitals need more PPE to handle [additional cases],” she said.
The country recorded more than 33,000 cases of COVID-19 as of Tuesday, with more than 1,900 deaths, government data show.