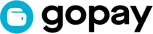Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultsInequality will make the next pandemic worse
Pandemics are coming faster and spreading more widely, threatening more lives and livelihoods than ever before.
Change text size
Gift Premium Articles
to Anyone
T
he science of fighting disease has never been stronger. We have the means to detect outbreaks immediately, sequence pathogens in the space of days and develop new vaccines in just months. Yet pandemics are coming faster and spreading more widely, threatening more lives and livelihoods than ever before.
Recall the trauma of COVID-19, which inflicted economic hardship on billions of people and caused an estimated 18.2 million excess deaths between Jan. 1, 2020, and Dec. 31, 2021. Public-health officials had previously warned of the likelihood of a pandemic, former United States president Barack Obama had responded by setting up a pandemic-preparedness office within the US National Security Council. But his successor, Donald Trump, dismantled it, leaving the US more exposed.
Once again, public-health officials are warning that another pandemic is a matter of “when, not if.” Yet despite the devastating effects of the last one, the world seems to have turned a blind eye to the issue.
The Global Council on Inequality, AIDS, and Pandemics, which we cochair, recently issued a report on this risk, in conjunction with the G20 meeting of health ministers in Johannesburg, South Africa. Using evidence from COVID-19, AIDS, Ebola and mpox, the report identifies a vicious cycle: inequality and its associated deprivations increase the chances of pandemics and deepen their effects; and pandemics increase inequality, often with devastating effects for the lowest-income people.
In the case of COVID-19, low-wage frontline workers typically suffered disproportionately, exhibiting a greater incidence of illness and hospitalization, partly because they could not retreat to Zoom meetings. And when they did fall ill, they had no choice but to dig into their meager savings.
Thus, addressing pandemics entails more than a medical response. We also must look at socioeconomic factors. Crowded living conditions, frontline occupations and poverty all contribute to the spread of pandemics, as do poor nutrition and baseline health characteristics. That is why countries with universal health-care systems did better during the COVID-19 crisis than those without. In the absence of such systems, economic inequality leads to health inequality.
Addressing inequality thus must be central to how we prepare for, and respond to, future pandemics, not just because caring for the vulnerable is the right thing to do, but also because it is the best approach overall. COVID-19 showed that when regions anywhere in the world did not have access to vaccines, therapeutics and protective gear, the disease festered and mutated, creating new risks for everyone. The “me-first” vaccine apartheid practiced by advanced economies was not only morally abominable; it was also self-defeating.