Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
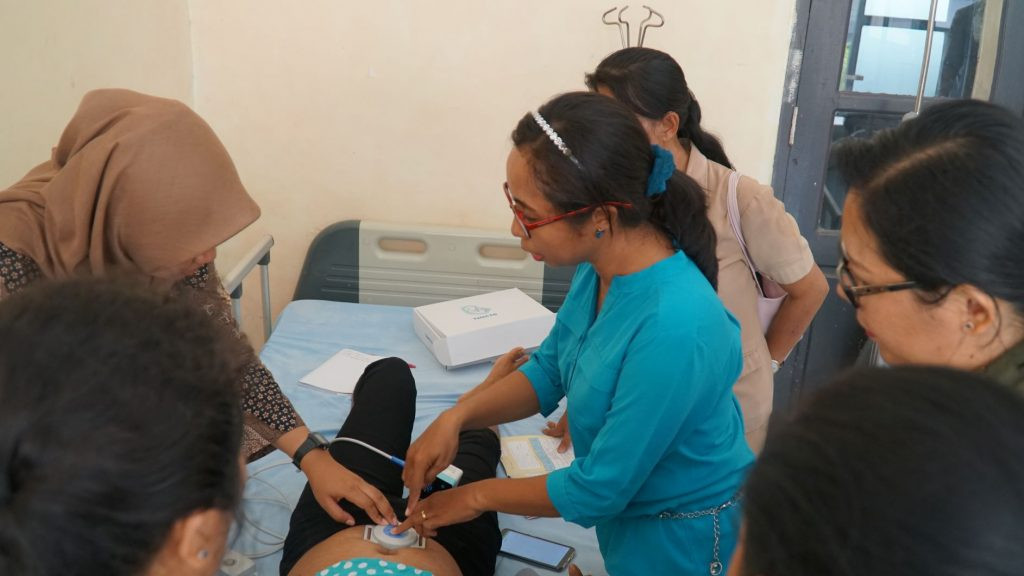
View all search resultsThe digital divide in basic health care: Obstacles in eastern Indonesia
In the remote regions of Eastern Indonesia, a rigid digital reporting system is forcing midwives to choose between ticking boxes and saving lives.
Change text size
Gift Premium Articles
to Anyone
“Which should we prioritize: serving the patients or inputting the data?” This question, posed by a midwife in the Rumah Tiga subdistrict, Ambon, Maluku, underscores a growing crisis in Indonesia’s healthcare system.
While the question may sound paradoxical, as clinical care and data entry are meant to be complementary, it reflects a harsh reality for healthcare providers in the nation’s outermost, furthest and most remote (3T) areas. For these midwives, the two services have become a Catch-22. If they focus on clinical care, their digital reporting is neglected; if they prioritize data entry, the quality of maternal and child health services is inevitably compromised.
The Ultralight Project 2024, a comprehensive research study focusing on the digitalization of maternal and child health (MCH) services in Ambon and Kupang regency, East Nusa Tenggara, offers a critical look at how these systems function in the field. All current governmental regulations, including Government Regulation No. 28/2024 that implements the 2023 Health Law, reiterate that a midwife’s duty centers on MCH services. This includes everything from routine check-ups to ensuring emergency referrals when complications arise. The goal of this framework is noble and clear: to drastically reduce the maternal mortality rate (MMR) and meet the ambitious United Nations Sustainable Development Goal of fewer than 70 deaths per 100,000 live births.
Midwives are undeniably on the front line of this mission, serving as the healthcare personnel closest to the community. However, their role is complicated by their dual identity. Within the organizational structure of the Indonesian healthcare system, midwives are also part of the state apparatus. This means they are bound by the same administrative obligations as any other civil servant, including the exhaustive requirement to keep digital records and submit real-time reports. In practice, this requires them to navigate a labyrinth of applications for patient registration, antenatal care, child development tracking and referral management.
Ideally, inputting data into these digital applications should be a simple precursor to providing medical services. In the 3T regions, however, this task is rarely completed in one go. Midwives are frequently stymied by systemic constraints such as extreme loading delays, software errors, signal interference and sudden power outages.
Furthermore, the system often requires a valid National Identification Number (NIK) to proceed. In remote regions, where many residents lack formal documentation or have invalid ID numbers, this creates a total deadlock. The midwife is then left with a choice: deny service to a patient in need, or provide the service and accept that the data, and thus their performance record, will remain incomplete.
This "double burden" of clinical service versus digital administration has led to a measurable decline in performance. Recent studies indicate that the service performance of midwives dropped to a low of 58.1 percent between 2021 and 2023, a figure that sits significantly below that of other health workers at community health centers (Puskesmas).