Popular Reads
Top Results
Can't find what you're looking for?
View all search resultsPopular Reads
Top Results
Can't find what you're looking for?
View all search resultshealth-insurance
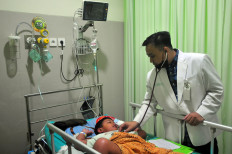
BPJS Kesehatan to use facial recognition in prevention of frauds
The state-owned Health Care and Social Security Agency (BPJS Kesehatan) is planning to use a facial recognition technology to identify millions of its policyholders and to prevent fraud in the National Health Insurance (JKN) system.
PREMIUM
Hospitals win, insurers lose as medical claims surge on rising costs
As the number of health claims rise, industry analysts are urging insurers and hospitals to review their risk-sharing schemes to avoid transferring the burden from the former to the latter, among other measures.
PREMIUM
Nearly 270 million Indonesians now covered by national health insurance
Coinciding with World Health Day, the Healthcare and Social Security Agency (BPJS Kesehatan) has announced that close to 270 million people, nearly the country’s whole population, have been enrolled in the National Health Insurance (JKN) program.
PREMIUM
Private insurers want limits to scope of public healthcare coverage
Analysts have urged finalizing the prolonged discussions over a Coordination of Benefits (COB) scheme, which they say will reduce public-private competition and ultimately help the government toward achieving its universal health coverage goal, alleviate risk for private insurers as well as ensure better health benefits for all.
PREMIUM
Government seeks to implement new JKN service classes for inpatient care
The government is working to implement new categories of inpatient coverage for National Health Insurance (JKN) in 2022, as part of its efforts to restructure benefits for policyholders and ensure the deficit-stricken program’s sustainability.